HealthTeamWorks partners with clients to design and implement workflows that optimize patient care and financial performance across payment models. We provide our network clients the expertise and the journey from volume-to-value and empower delivery system changes, provider collaboration and market leading improvements to achieve the 5-Part Aim: increased clinical quality, lowered costs, improved patient experience, workplace satisfaction, and thriving healthcare businesses.
Clinical and operational integration across the continuum of patient services is essential for high-performing networks to deliver cost-efficient, high quality care, and to manage population health under fee-for-service and value-based payment contracts. Our approach fosters sustainable improvement for organizations providing: advanced primary care thought-leadership and implementation, development of high-performing accountable care networks, and leadership and support of programs that operate on the regional, national and international levels.
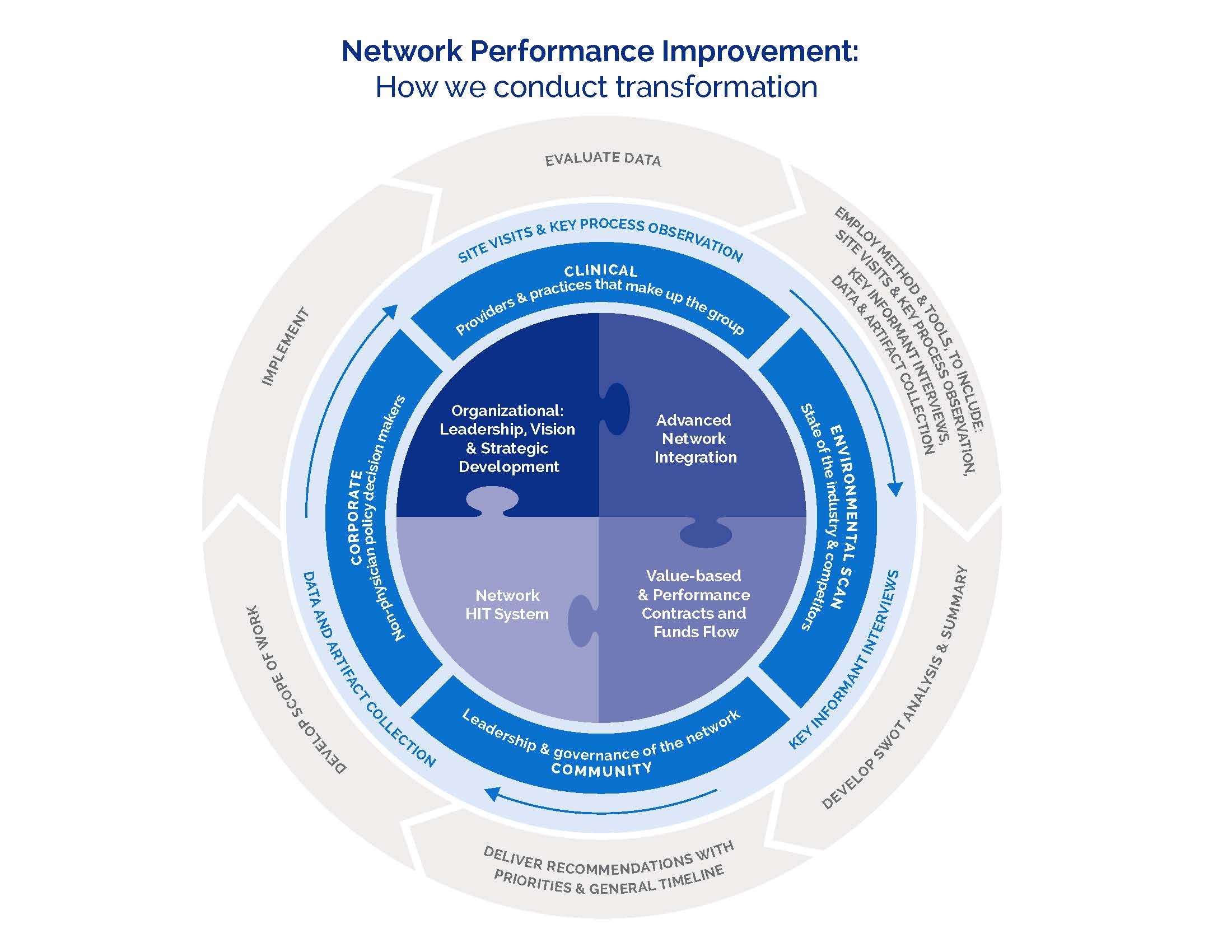
Integrated Delivery Network Evaluation Matrix
IDN Organization, Leadership, Vision, & Strategic Development
5-Part Aim organizational competency is built upon a foundation of IDN leadership, organizational infrastructure and member accountability designed to deliver on short and long-term marketrelevant value.
IDN Physician Governance, Bylaws, Membership and Services Agreements, Articles of Incorporation; key Committees (Clinical HIT, Value Performance, Finance, Contracting, Membership).
Key IDN Policies (Member Participation, HIT, Security & HIPAA, Contracting, Network Management)
designed for 5-Part Aim effectiveness/ transparency, meaningful membership participation, fees &
accountability.
Primary Care foundation (>50% general & Board membership) & Leadership positions (IDN and key
committee chairs) with ~50% PCP Governance membership.
Dyad Executive leadership (physician and business) with an administrative & management team
supporting IDN domains (PI & APC, clinical HIT, analytics, contracting, membership).
Membership Segmentation: by IDN role (PCP, Primary SCP, Tertiary SCP and Facilities, BH) and IDN engagement (transformation status, engagement, performance, payer contract and IDN organizational participation) --defines IDN support level/benefits, funds flow, value proposition.
Dramatic, comprehensive, and imperative changes are required of the healthcare industry to solve for the explosive, low-value cost of care. A high-performing IDN must have organizational competencies for data-driven, deep, and real-time understanding of the healthcare work provided, and the ongoing capacity for iterative learning, adaptation, and change.
Governance and strategic commitment (strategic and tactical design, funding, staffing) to Learning Organization infrastructure and systems: performance improvement science, practice transformation support, data-powered collaborative learning.
Operational IDN performance improvement system properties: 1) Value Performance (quality) Charter and work plan with 5-Part Aim focus, 2) staffing to include practice transformation coaches and PI subject matter experts and 3) transformative clinical analytics and 4) practice-level systems and culture of advanced teamwork and continuous performance improvement.
Near term strategy and tactics designed for stakeholder engagement ("meeting them where they are at") with explicit value propositions/business cases that include multi-year implementation, participation, IDN support and accountability glide paths. Key Stakeholders include PCPs, Primary SCPs, Tertiary SCPs and Acute Care Facilities, Payers, and Employers.
Formal collaboration structure and accountability for PI and Analytics teams around analytics tools designed to promote high-functioning teamwork and healthcare worker and patient behavior change.
IDN and practice performance measures optimized for relevance to network value-based payment initiatives and to the 5-Part Aim work of provider teams and other IDN providers.
The worsening prevalence of 'burnout' in primary care, now ranging from 50-60%, requires urgent diagnosis and treatment. It reflects both the inherent emotional burdens of empathic clinical work and the growing work-life toxicities of modern systems of healthcare: for instance, FFS economics that prioritize "RVU" production over quality of care, the intrusion of electronic documentation into the physician-patient relationship, the market demands for transparent value (which, while sensible, are out in front of current practice capabilities). Additionally, the imperative of practice transformation, to 'advanced primary care,' represents a further challenge for providers and their teams. The vitality of work--meaning and purpose--is threatened, particularly for front-line, primary care providers. To attract and grow healthy advanced primary care practices, IDN strategic planning must prioritize comprehensive changes in organizational structure, systems of care, provider/team roles and responsibilities, payment models (transition from FFS to value-based compensation) and the culture of 'medical practice' itself.
Formal IDN leadership commitment to the ongoing measurement, understanding and improvement of provider/team work experience as a function of organizational and practice design.
Design principles for meaningful clinical work: top of license work, prepared team, patient relationship centered, workflow efficiency & Muda elimination (health information technology and advanced teamwork), performance effectiveness, & pay (at the individual, team and practice levels) commensurate with IDN 5-Part Aim performance impact.
IDN organizational and operational platform(s) for meaningful provider/team voice to inform improvement of IDN functional design and care delivery.
The economic and cultural models of healthcare practice are firmly entrenched as 'silos.' No matter how strong the business case or leadership, the magnitude of change required of traditional systems of healthcare are formidable and will take years. Therefore, it is imperative that both the near and long-term promise and vision for IDN collaboration, along with realistic stages of organizational development, are well designed and articulated.
Leadership commitment to long-term vision and strategic organizational development required for 1) best-of-class 5-Part Aim performance, and 2) thriving business models for both the IDN and its member practices. This commitment includes milestones for infrastructure and services development, measures of accountability and sustainable resourcing. Near-term strategy and tactics for IDN 5-Part Aim impact (key organizational competencies in VBP marketplace).
Near term strategy and tactics for IDN 5-Part Aim impact (key organizational competencies in VBP marketplace).
Near term strategy and tactics designed for stakeholder engagement ("meeting them where they are at") with explicit value propositions/business cases that include multi-year implementation, participation, IDN support and accountability glide paths. Key Stakeholders include PCPs, Primary SCPs, Tertiary SCPs and Acute Care Facilities, Payers, and Employers.
Prioritized network infrastructure development that includes near and long-term implementation, funding, and sustainability models. Examples of key network infrastructure: clinical and claims data analytics, risk stratified care management, strategic allocation of support services (centralized and embedded), practice transformation coaching, HIT utility model.
Cultural integration through compelling value propositions & participation requirements for all IDN stakeholders, 5x/5-way communication program (web-based tools/virtual collaboration site, newsletters etc.), IDN process and performance socialization (e.g., membership, committee meetings; story boards, best-practice testimonials).
IDN commitment to and investment in physician leadership development including executive and management skills.
IDN consulting and collaboration resources to support practice-level business management best practices (e.g., business model, financial management, HR, billing, and collections).
Advanced Network Integration
Advanced Network Integration: The primary driver of patient (and employer)-centric value--quality, experience, and cost of care--is the degree of provider integration and alignment around 5-Part Aim performance at the regional healthcare system level.
IDN navigation services policies, staffing, support and HIT functionality designed to optimize collaborative patient care across the network and associated communities.
Network integration measurement, standards, and reports: network referral integrity, PCP/SCP provider access (TTT appointment), care compact completion and performance, level of care and loop closure, adherence to care pathways and co-management protocols, and the measurement the efficiency, effectiveness and experience (both patient and provider) of team-based clinical care across the network.
Development and recruitment of IDN healthcare (medical) members who excel in high-functioning networks (collaborative/ coordinated systems of care) including PCPs, Primary SCPs, inpatient, lab/imaging, Extended Care Facilities (ECF), Urgent Care Center (UCC) etc.
Network development of and integration with behavioral health, clinical pharmacology /MTM, and non-medical community-based resources (Community Based Organizations/CBO) through community health workers/health navigators and Community-Clinical Linkages.
Advanced primary care is essential--but insufficient--for the population-health performance accountabilities of an IDN. Expansion of the advanced primary care model and team, to become a "system property of the community,' is vital to understand the "lived" environment of high risk, high cost patients, and to effectively impact both population and public health/SDOH performance.
IDN development of community-based APC team members, such as Health Navigators/Community Health Workers, to power engagement of at risk/high risk patients, support care collaboration/navigation, 'lived environment' assessment and SDOH-informed care plan, community-clinical linkages, patient activation and preparation.
Hot Spotter analytics to inform the clinical work of APC & health navigators (including PSDOH assessment, coordination, and navigation of community-clinical linkage services).
Community Integrated Primary Care workforce development: new skills, accountabilities, roles (such as Health Navigator, Population Health Specialist).
Palliative care integrated into IDN and APC services as key patient-centered resource (especially home-based palliative care -HBPC- ).
High-value population health management requires a foundation of high-performing, team-based primary care powered by high-value clinically relevant data analytics and IDN support services (including PI, coaching, HIT); effective patient-centered care across the network also requires specialty care providers/practices develop high-functioning teams (and other best practices of APC).
IDN strategic prioritization, infrastructure support and workforce development for advanced primary care as the standard network model for primary care.
Advanced teamwork model ("APC," based on Bodenheimer's 10 Building Blocks): collaborative, prepared, proactive, TOL roles, data-powered; patient (PFAC) and network integration; teamlet staffing; advanced access & non-visit care (telehealth, eVisits); practice leadership (champion & sponsor).
Resources and support for development of advanced systems of practice (both primary and specialty care), ongoing performance improvement and data engagement facilitated by practice transformation coaches; practice performance and best practices routinely shared across the network.
Direct Primary Care development and IDN support based on a hybrid, APC-integrated model ("Integrated Direct Primary Care"--DPCi).
Advanced Primary Care workforce and support development: new skills, accountabilities, roles (such as advanced MA, practice transformation coaches).
VALUE BASED, IDN PERFORMANCE PAYER CONTRACTS AND FUNDS FLOW
The organizational, system and accountability transformations required of an effective IDN requires a new, network-wide business model and associated novel funds flows (supporting practice/network transformation, governance and IDN operations and ongoing and novel IDN support services).
VB-contracts, both CMS and commercial payer, for empaneled patients (designed to delivery on and reward 5-Part Aim performance) and with Board-directed requirements for IDN member participation. CMS and commercial quality program/contract analysis, alignment, prioritization participation, credentialing, and support strategy.
VB contract funds flow to support IDN administration, management and infrastructure including IDN support services, staffing, leadership, VB payer contracting and new workforce roles.
VB Payer Contracts funds flow to power APC practices, clinical home care, palliative medicine, and behavioral health.
VB Payer Contracts funds flow to reward specialty care and tertiary care providers for efficient/effective/ coordinated clinical services.
IDN funds flow to support non-medical community resources that are central to CIPC.
Integrated DPC (DPCi) direct to employer (DTE) business model and funds flow to support APC & IDN infrastructure.
The Economic Denominator Principle of value-based healthcare means an IDN must deliver on the prime directive of lower 'total cost of care' and premiums (for patients & employers) while demonstrably improving quality of care, access, patient experience, and provider/staff vitality.
Mission, strategic and operational commitment to TCOC efficiency & the mitigation of structural, work-effort, human resource, and operational Muda.
IDN investment in and development of critical, high value services/systems/human resources (e.g., APC, palliative medicine, CIPC, patient-centered care navigation, stewardship, and care efficiency analytics).
IDN divestment and proactive transitions from critical low value, high Muda (FFS payment models, volume-based services, low value providers/procedures, out-of-network services).
Systematic and standardized use of claims/utilization analytics and measures to assess provider efficiency (quality, use of resources, appropriate testing, cost, referral patterns and loop closure), identify low value & high Muda services, and inform and empower IDN members and support systems in efficiency optimization.
Narrow network of affordable high-quality providers/facilities beyond the IDN (for services not available within the IDN).
NETWORK HIT SYSTEM
The fundamental power of an IDN is the collaborative efficiency & effectiveness of integrated delivery--this principle must be applied to the IT/IS tools that are critical to clinicians' patient care, information integration across the network and transformative clinical analytics: health information technology. (The corollary is to reject the 'acceptance' of bad system engineering and HIT fragmentation as 'normal'--and to "just say no" to lipstick-on-a-pig approach to HIT.)
IDN strategic commitment to practice HIT optimization, across all specialties and other community providers, with a bias towards computer factor engineering (over human factor engineering) to support best practice clinical & network workflow efficiency, clinical data acquisition, transformative data analytics and 5-Part Aim effectiveness.
Long term IDN HIT operational structure to include HIT system ownership and control, service, and support accountability (database, development, clinical workflow optimization support, training, vendor management, HIE integration).
IDN commitment and glide path towards community-based EHR utility model: single instance, common database; centralized support with local development, upgrade, vendor management and training resources; economies of scale; and best-practice clinical/teamwork workflow efficiencies ("pull strategy").
Network HIT executive physician leadership
The healthcare system output required by the market, and its demand for transparent Triple Aim performance, is data; to excel in this output, high performing IDNs must empower its frontline workers (physicians and their teams) with data and data tools (as in the Toyota Production System).
IDN ownership of clinical and claims data & analytics (enterprise database and analytics tools) with IDN management, development, training, and support.
IDN clinical data analytics with data tools designed to power advanced teamwork, practice transformation coaching, performance improvement and Community Integrated Primary Care (huddle, universal registries, risk stratification, network optimization, utilization, patient & provider experience).
Claims data payer-partnerships for IDN analytics--concurrent utilization data, reports and sharing across all empaneled populations
Direct Primary Care development and IDN support based on a hybrid, APC-integrated model ("Integrated Direct Primary Care"--DPCi).
IDN 5-Part Aim measure library: clinical and utilization measure standardization, maintenance, and reporting; strategic use of transparency with benchmark comparison (peer, group, and national); performance reports designed for end-user access, optimized for behavior change; and IDN measures optimized for national and regional value-based payment initiatives.
